The Mechanics of Screwless Dental Implants: Structural Innovations in Restoration
Screwless dental implants represent a significant shift in restorative dentistry, moving away from conventional threaded systems toward friction-fit and press-fit mechanisms. These innovations eliminate mechanical bolts, relying instead on controlled pressure and bioactive surfaces to achieve stability. The structural changes influence bone integration, load distribution, and long-term maintenance. Understanding the procedural mechanics, biological responses, and clinical applications of threadless designs provides insight into how these systems function and where they may offer distinct advantages in specific anatomical contexts.
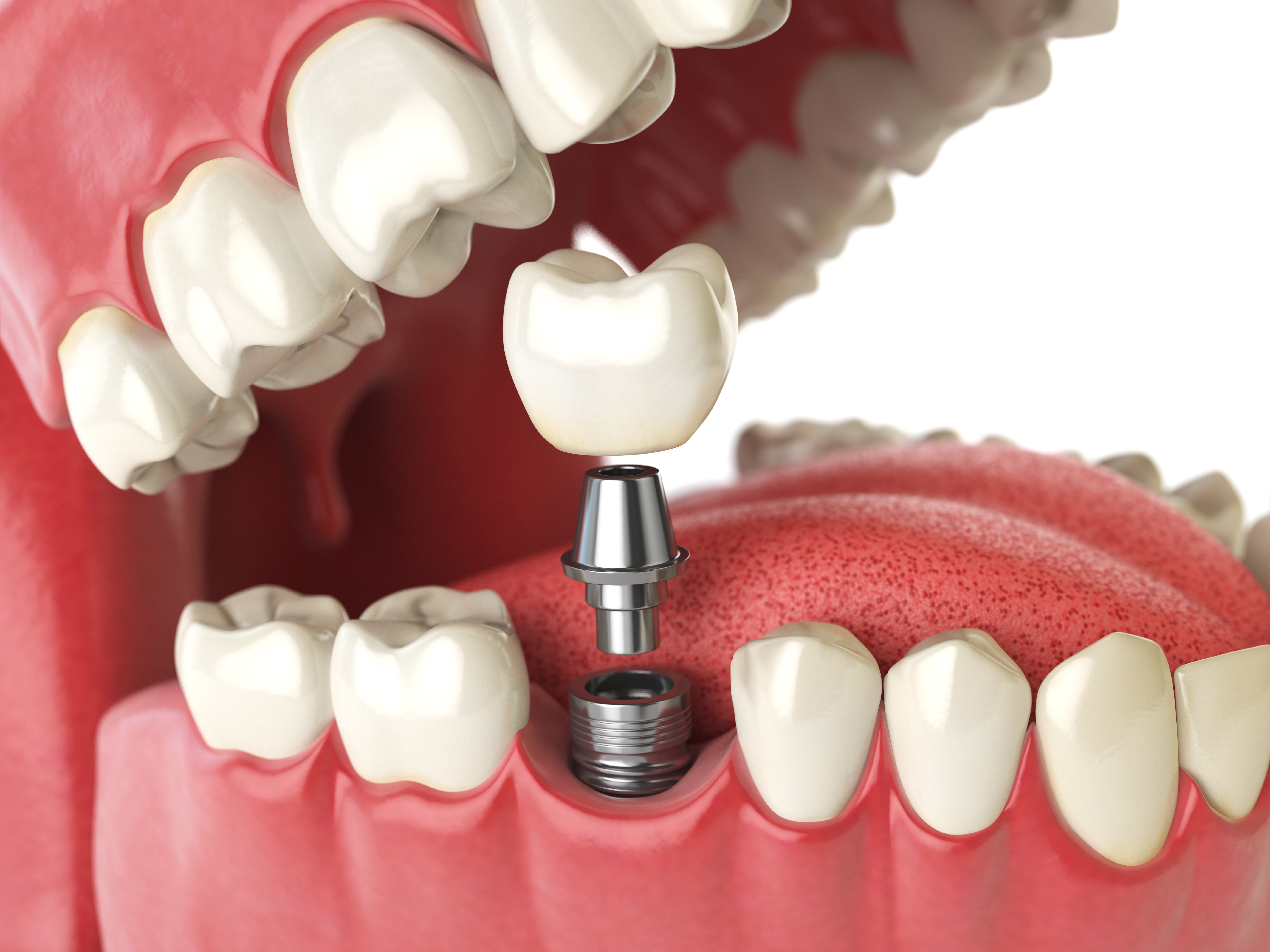
Dental implant technology has evolved considerably over recent decades, with researchers and manufacturers exploring alternatives to conventional threaded designs. Screwless implants challenge traditional assumptions about how artificial tooth roots should interact with bone tissue, offering different mechanical properties and clinical workflows.
How Friction-Fit Mechanisms Secure the Prosthetic Without Mechanical Bolts
Friction-fit systems rely on precise engineering tolerances to create retention between implant components. The abutment or prosthetic element fits into the implant body with carefully calculated dimensions that generate sufficient friction to resist displacement forces during function. This interference fit depends on the elastic deformation of materials at the connection interface, creating a mechanical lock without threads or screws.
The taper angle at the connection point plays a critical role in determining retention strength. Steeper tapers generally provide stronger friction but may complicate component insertion and removal. Manufacturers typically use angles between 5 and 15 degrees to balance these considerations. Material selection also influences friction characteristics, with different combinations of titanium alloys, zirconia, or other biocompatible materials producing varying retention forces.
Some friction-fit designs incorporate additional features like micro-ridges or textured surfaces at the connection interface to enhance grip. These microscopic elements increase the effective surface area and create additional mechanical interlocking points. The absence of screw access channels in these systems can provide aesthetic advantages in anterior restorations where translucency matters.
Evaluating the Structural Differences in Press-Fit Technology
Press-fit implants differ fundamentally from threaded designs in how they engage surrounding bone. Rather than cutting into tissue during placement, these systems compress bone laterally as they are inserted into a precisely prepared osteotomy. The preparation protocol typically creates a site slightly smaller than the implant diameter, requiring controlled force to seat the implant fully.
This compression generates immediate primary stability through radial pressure against the bone walls rather than mechanical threading. The stress distribution pattern differs from threaded implants, with forces concentrated at the implant periphery rather than along spiral threads. Some research suggests this may influence how bone remodels around the implant during the healing phase.
Press-fit designs often feature cylindrical or slightly tapered geometries with smooth or minimally textured surfaces. The lack of threads means these implants rely entirely on friction and bone compression for initial stability, which may affect their suitability for different bone densities. Softer bone types may not provide adequate resistance to micromotion, while dense bone may complicate insertion.
The Role of Bioactive Surfaces in Accelerating Bone Integration
Surface treatments become particularly important for screwless implants since they lack the mechanical advantage of threads during the healing period. Bioactive coatings and surface modifications aim to promote faster and more complete osseointegration by encouraging cellular activity at the bone-implant interface.
Hydroxyapatite coatings represent one common approach, providing a calcium phosphate layer that mimics natural bone mineral composition. These coatings can stimulate osteoblast attachment and proliferation, potentially reducing healing times. Other surface treatments include acid etching to create micro-roughness, sandblasting with biocompatible particles, or plasma spraying to deposit bioactive materials.
Some advanced systems incorporate growth factors or peptide sequences designed to attract bone-forming cells specifically. These biochemical signals can complement the mechanical properties of the implant, creating conditions favorable for rapid integration. The effectiveness of these treatments varies based on application methods, coating thickness, and individual patient factors like bone quality and systemic health.
Analyzing How the Absence of Threads Alters Load Distribution Across the Jawbone
Threaded implants distribute occlusal forces along the spiral thread pattern, creating stress concentrations at thread peaks and valleys. Screwless designs eliminate this specific stress pattern, instead transferring loads more uniformly across the implant-bone interface. This altered biomechanical behavior has implications for long-term bone maintenance and implant survival.
Finite element analysis studies have examined stress distribution in threadless implants under various loading conditions. Results suggest that smooth cylindrical implants may concentrate stresses at the crestal bone region, potentially leading to different patterns of bone resorption compared to threaded designs. The absence of threads means forces cannot be distributed along a helical path, requiring alternative mechanisms to dissipate functional loads.
The implant diameter and length become even more critical for threadless designs since surface area directly determines load-bearing capacity without the additional engagement provided by threads. Wider or longer implants may be necessary in some clinical situations to achieve adequate stress distribution. The elastic modulus of the implant material also influences how forces transfer to surrounding bone, with stiffer materials potentially creating stress shielding effects.
The Procedural Mechanics of Preparing the Site for Threadless Insertion
Site preparation for screwless implants requires exceptional precision since the osteotomy must match the implant dimensions closely to achieve proper friction-fit retention. Drilling protocols typically use sequential diameter increases with final dimensions determined by bone density measurements. Dense bone may require preparation to exact implant diameter, while softer bone might benefit from slight under-preparation to enhance compression.
Depth control becomes critical to ensure complete seating without excessive insertion force that could damage surrounding structures. Many systems include depth gauges or stops to guide preparation. The osteotomy walls should be smooth and parallel or slightly tapered to match the implant geometry, requiring careful drilling technique to avoid irregularities that could compromise fit.
Some threadless systems use specialized insertion instruments that apply controlled force while monitoring torque or displacement. These tools help clinicians achieve proper seating without exceeding safe limits that could fracture bone or deform the implant. The insertion pathway must be carefully planned to avoid critical anatomical structures like nerves, blood vessels, or sinus cavities, with imaging guidance often employed for complex cases.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
Conclusion
Screwless dental implants demonstrate how engineering innovation continues to expand treatment options in restorative dentistry. By eliminating traditional threads and mechanical fasteners, these systems offer alternative approaches to achieving stability and osseointegration. The friction-fit mechanisms, specialized surface treatments, and modified load distribution patterns represent distinct biomechanical strategies that may suit specific clinical scenarios. As research continues to evaluate long-term outcomes, these structural innovations contribute to the broader evolution of implant technology and surgical techniques.




